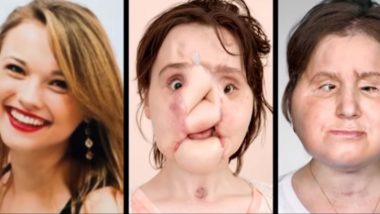
Facial transplantation once existed only within the realms of science fiction and fantasy. But today, it has moved from being an experimental possibility to a medical reality, giving new lease of life to many victims of facial disfigurements. In the recent news is the story of Katie Stubblefield, a 22-year-old girl who lost a substantial part of her face to a self-inflicted rifle shot in 2014. Tragically, the suicide attempt failed, leaving her severely maimed with a large portion of her face blown away.
Two years after the tragedy, the Stubblefield family finally had something to smile about. Katie finally found a match for a face transplant -- 31-year-old Adrea Schneider who died of a drug overdose. Today, more than a year after her surgery, Katie finally has a new face and has found a semblance of normalcy in life after the tragic accident.
What is Face Transplant?
Face transplant, as the name suggests, is a medical procedure where the facial tissues from a cadaver are donated to a person whose face may be disfigured congenitally or through trauma. According to John Hopkins Medicine, it is an operation which involves the transplantation of skin, muscles, nerves, blood vessels and bone. It may also include some parts of the scalp and skull, all the way down to the jaw and chin.
Kate is the 40th patient in the world and at 21, the youngest in the US to have received a face transplant. Before her, there have been a few notable cases, including that of Li Guoxing from China whose face was disfigured during a bear attack and Dallas Wiens from the US who lost portions of his face after being electrocuted.
What Does Face Transplant Entail?
The human face is an intricate arrangement of layers of skin, hair and muscles, blood vessels, nerves, cartilage and bone. It facilitates essential functions like eating, tasting, smelling, apart from helping humans communicate through verbal and non-verbal gestures. The face is what gives a person his or her distinct identity and in an image-conscious society, any disfigurement to the face can extensive psychological and emotional stress to the sufferer.
That's why victims of extensive facial disfigurement are often considered for face transplant since it is important for their physical, psychological and social well-being.

Who is Eligible for Facial Transplant?
John Hopkins Medicine states that not everyone with facial malformations is eligible for facial transplant. People who have suffered extensive facial malformation can consider facial transplants. To be eligible, the person should be between 18 to 60 years of age, suffering from facial disfigurement. The patient should have no history of cancer for at least five years, HIV or Hepatitis C; and ability to take immunosuppressants. If the candidate is a woman, she should be willing to put pregnancy on hold for at least a year.
The Surgery
There may be a long wait involved till a perfect donor who matches the recipient's skin tone, blood type and tissue type is found. The surgery itself may take 12-36 hours, depending on the extent of the damage. The transplant itself will require a lot of precision-oriented microsurgeries to lift the donor's tissues, muscles, cartilage, and skin to place it on the recipient's face.
Surgeons may be grouped into a team of two. One team will work towards peeling away the face from the dead donor and the second team will prep the recipient to receive the donor's face. The team will then painstakingly re-attach every artery, vein and nerve in the face.
What Are The Risks?
Face transplant can help improve the quality of lives of many victims of facial disfigurement. But the procedure is not as easy as it seems. Immediate risks include bleeding, infection, slow wound healing, pain and blood clots. The recipient may reject the donor's face since it is an "alien" tissue to the body. So in the long run, the patient may have to take a steady stream of immunosuppressing drugs to prevent the immune system from attacking the new face. These drugs pose additional health risks such as infection, diabetes, cancers, kidney damage and heart diseases.
Face transplant patients may also require extensive rehabilitation to help them regain some of their functions such as moving, eating, drinking and smiling. The donor's family often expect to see their deceased loved one in the face of the recipient but set themselves up for disappointment. In many cases, the human recipient may not resemble the donor because the shape of the face is largely determined by the underlying bone structure.
That being said, face transplant has helped numerous victims of facial disfigurement have a life of dignity instead. Kate Stubblefield's story may offer a ray of hope to many like her who live with partial or complete disfigurement.
(The above story first appeared on LatestLY on Aug 16, 2018 09:44 PM IST. For more news and updates on politics, world, sports, entertainment and lifestyle, log on to our website latestly.com).













 Quickly
Quickly